What to Eat During Pregnancy for the Health of Mother and Baby | Edwin Ogie Library
What to Eat During Pregnancy for the Health of Mother and Baby
Medical Disclaimer
This article is for educational and informational purposes only. It does not constitute medical advice, diagnosis, or treatment. The content presented here is compiled from publicly available health resources and reputable medical organizations. Always consult a qualified healthcare provider—such as your obstetrician, midwife, or registered dietitian—before making any dietary changes during pregnancy. Individual nutritional needs vary based on health status, pre-existing conditions, and stage of pregnancy.
Understanding Pregnancy Nutritional Needs

During pregnancy, your body undergoes remarkable changes to support the growing baby. According to the American College of Obstetricians and Gynecologists (ACOG), while caloric needs increase, the focus should be on nutrient density rather than simply eating more. The common phrase "eating for two" can be misleading—most pregnant women need only modest increases in calories.
- First Trimester: No additional calories needed for most women
- Second Trimester: Approximately 340 extra calories per day
- Third Trimester: Approximately 450 extra calories per day
- Multiple Pregnancy: Higher caloric needs—consult your healthcare provider
These are general estimates. Individual needs vary based on pre-pregnancy weight, activity level, and metabolic factors. Always consult your provider for personalized recommendations.
Essential Nutrients and Their Food Sources
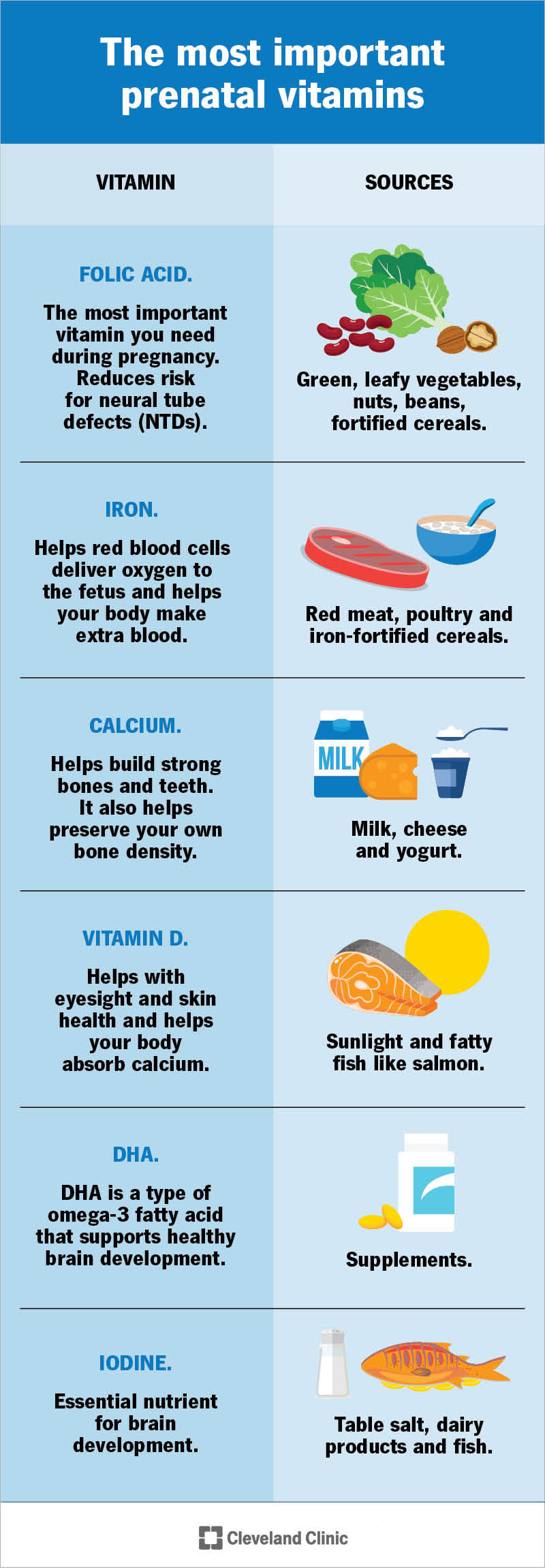
The Cleveland Clinic and other major health organizations emphasize several critical nutrients during pregnancy. Understanding these nutrients helps you make informed food choices.
- Folic Acid (Folate): The CDC recommends 400-800 mcg daily. Found in leafy greens, fortified cereals, beans, and citrus fruits. Critical for neural tube development.
- Iron: Needed for increased blood volume. Found in lean red meat, poultry, beans, spinach, and iron-fortified cereals. Vitamin C enhances absorption.
- Calcium: Supports fetal bone and teeth development. Found in dairy products, fortified plant milks, leafy greens, and tofu.
- Protein: Essential for fetal tissue growth. Found in lean meats, poultry, fish, eggs, beans, lentils, nuts, and dairy.
- Omega-3 Fatty Acids (DHA): Supports brain and eye development. Found in fatty fish (salmon, sardines), walnuts, flaxseeds, and fortified eggs.
- Vitamin D: Aids calcium absorption and immune function. Found in fortified milk, fatty fish, and through safe sun exposure.
- Iodine: Important for thyroid function and brain development. Found in iodized salt, dairy, and fish.
- Choline: Supports brain development. Found in eggs, meat, fish, and cruciferous vegetables.
Best Foods to Eat During Pregnancy

Building your diet around whole, nutrient-dense foods provides the foundation for a healthy pregnancy. The following food groups are generally recommended by nutrition experts and health organizations.
- Leafy Green Vegetables: Spinach, kale, broccoli, and Swiss chard provide folate, iron, calcium, and fiber
- Lean Proteins: Chicken, turkey, lean beef, eggs, beans, lentils, and tofu support fetal growth
- Whole Grains: Oats, quinoa, brown rice, and whole wheat provide B vitamins, fiber, and sustained energy
- Fruits: Berries, oranges, bananas, apples, and avocados offer vitamins, minerals, and natural sugars
- Dairy or Fortified Alternatives: Milk, yogurt, cheese, or fortified soy/almond milk for calcium and protein
- Fatty Fish: Salmon, sardines, and trout (2-3 servings per week) for omega-3 fatty acids
- Nuts and Seeds: Walnuts, almonds, chia seeds, and flaxseeds for healthy fats and minerals
- Legumes: Lentils, chickpeas, and black beans for plant-based protein, iron, and folate
- Sweet Potatoes: Rich in beta-carotene (converts to vitamin A), fiber, and potassium

Foods to Limit or Avoid
Food safety is particularly important during pregnancy because hormonal changes can weaken the immune system. Additionally, certain foods may contain substances that could affect fetal development.
- Raw or Undercooked Animal Products: Raw sushi, undercooked eggs, and rare meat may contain harmful bacteria (salmonella, listeria, toxoplasma)
- Unpasteurized Dairy and Juices: These may harbor listeria bacteria
- High-Mercury Fish: Shark, swordfish, king mackerel, tilefish, and bigeye tuna. The FDA recommends limiting albacore tuna to 6 ounces per week
- Deli Meats and Hot Dogs (unless heated): Potential listeria risk
- Refrigerated Pâtés and Meat Spreads: Listeria concerns
- Raw Sprouts: Alfalfa, clover, and radish sprouts may harbor bacteria
- Excess Vitamin A: Avoid high-dose vitamin A supplements and excessive liver consumption
- Alcohol: The CDC and Surgeon General recommend complete abstinence—no known safe amount
- Caffeine: Most organizations recommend keeping intake below 200mg per day (approximately one 12-oz cup of coffee)
- Processed and Junk Foods: High in empty calories, sodium, and unhealthy fats with minimal nutritional value
- Added Sugars: Excessive sugar intake may contribute to excessive weight gain and gestational diabetes risk
- Sodium: High sodium intake may contribute to swelling and blood pressure issues
- Wash all fruits and vegetables thoroughly under running water
- Keep raw and cooked foods separate to prevent cross-contamination
- Cook meats to safe internal temperatures
- Refrigerate leftovers promptly (within 2 hours)
- Check expiration dates on all packaged foods
Hydration During Pregnancy

Proper hydration is essential during pregnancy. Water helps form amniotic fluid, aids nutrient transport, supports digestion, and helps prevent common pregnancy complaints such as constipation and urinary tract infections.
- The Institute of Medicine recommends approximately 10 cups (2.4 liters) of total fluids daily from all sources during pregnancy
- Water should be the primary beverage choice
- Increase fluid intake during hot weather, physical activity, or illness
- Limit sugary drinks and monitor caffeine-containing beverages
- Carry a reusable water bottle as a visual reminder
- Drink a glass of water with each meal and snack
- Include water-rich foods: cucumbers, watermelon, oranges, strawberries, and soups
- Monitor urine color—pale yellow generally indicates adequate hydration
- If plain water is unappealing, add lemon, lime, mint, or cucumber slices
- Herbal teas may be hydrating, but check with your provider regarding specific herbs
Meal Planning and Portion Guidelines

The "My Pregnancy Plate" model, adapted from general healthy eating guidelines, provides a visual framework for balanced meals. Rather than strict calorie counting, this approach focuses on proportions and food quality.
- Half your plate: Non-starchy vegetables (spinach, broccoli, peppers, carrots)
- One-quarter: Lean protein (chicken, fish, beans, tofu, eggs)
- One-quarter: Whole grains or starchy vegetables (brown rice, quinoa, sweet potato)
- Plus: A serving of fruit and dairy or fortified alternative
- Healthy fats: Avocado, olive oil, nuts, and seeds in moderation
- Greek yogurt with berries and nuts
- Apple slices with almond butter
- Whole grain crackers with cheese
- Hummus with vegetable sticks
- Hard-boiled eggs
- Trail mix with dried fruit and seeds
Managing Pregnancy Cravings
Food cravings are common during pregnancy and are generally considered normal. However, managing them mindfully helps maintain nutritional balance and healthy weight gain.
- Craving sweets? Try fresh fruit, yogurt with honey, or a small piece of dark chocolate
- Craving salty foods? Opt for lightly salted nuts, popcorn, or whole grain crackers with hummus
- Craving ice cream? Try frozen yogurt, banana "nice cream," or a fruit smoothie
- Craving crunchy textures? Choose raw vegetables, apple slices, or roasted chickpeas
- Keep healthy snacks readily available to avoid impulsive less-healthy choices
- Stay hydrated—sometimes thirst is mistaken for hunger
- Practice mindful eating: enjoy treats in moderation without guilt
Vegetarian and Vegan Pregnancy Nutrition
According to the Academy of Nutrition and Dietetics, well-planned vegetarian and vegan diets can be nutritionally adequate during pregnancy. However, certain nutrients require special attention.
- Protein: Combine legumes, tofu, tempeh, nuts, seeds, and whole grains throughout the day
- Vitamin B12: Found naturally only in animal products—supplementation is typically necessary for vegans
- Iron: Plant-based iron (non-heme) is less readily absorbed. Consume with vitamin C-rich foods to enhance absorption
- Calcium: Fortified plant milks, tofu, leafy greens, almonds, and tahini
- Omega-3s (DHA): Algae-based supplements are recommended as plant sources (flax, chia) provide ALA, not DHA
- Zinc: Legumes, nuts, seeds, and whole grains
- Iodine: Iodized salt and seaweed (in moderation due to variable iodine content)
Common Nutritional Concerns
Many pregnant women experience conditions that affect eating and nutrition. Understanding these challenges and their dietary management can help you navigate them more comfortably.
- Eat small, frequent meals rather than large ones
- Keep bland snacks (crackers, toast) by your bedside and eat before getting up
- Avoid strong smells and greasy or spicy foods if they trigger nausea
- Ginger (tea, candies) may help some women—discuss with your provider
- Cold foods may be better tolerated than hot foods
- Stay hydrated with small sips throughout the day
- Eat smaller, more frequent meals
- Avoid lying down immediately after eating
- Limit trigger foods: spicy, fatty, acidic, and caffeinated items
- Elevate the head of your bed slightly
- Chew food thoroughly and eat slowly
- Increase fiber intake gradually: fruits, vegetables, whole grains, and legumes
- Drink plenty of water throughout the day
- Include prunes or prune juice, which may have natural laxative effects
- Stay physically active as approved by your provider
Sample Weekly Meal Plan
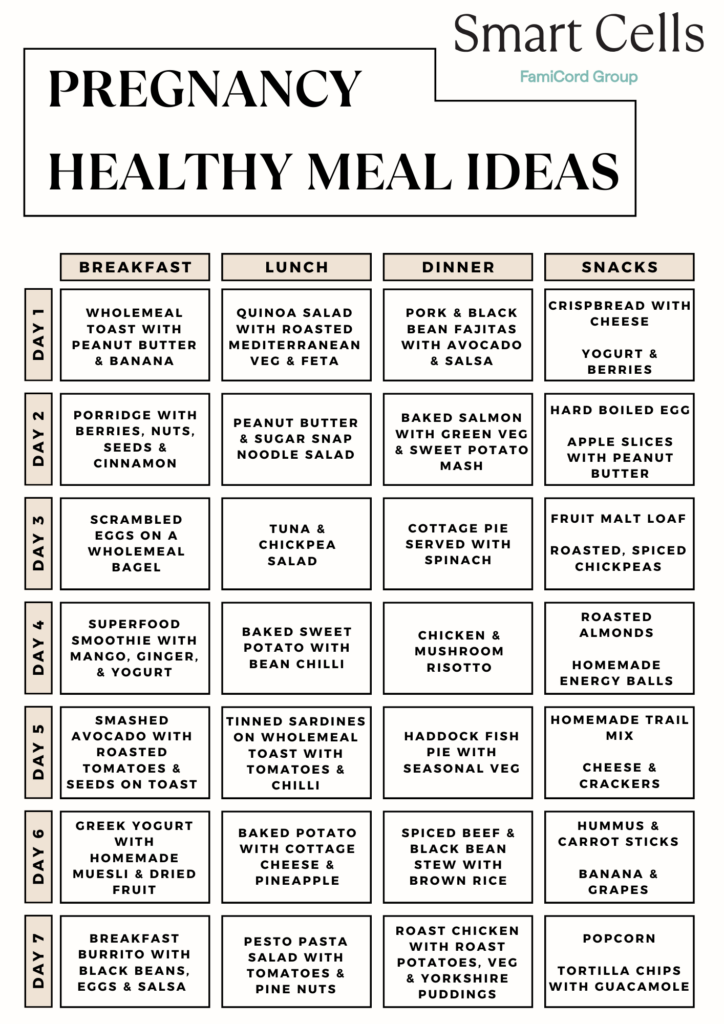
This sample meal plan provides general ideas based on nutritional guidelines. Adjust portions and choices according to your individual needs, preferences, and your healthcare provider's recommendations.
- Breakfast: Oatmeal topped with berries, chia seeds, and a drizzle of honey; glass of fortified milk
- Mid-Morning Snack: Greek yogurt with sliced banana and a handful of almonds
- Lunch: Grilled chicken salad with mixed greens, cherry tomatoes, avocado, quinoa, and olive oil dressing; whole grain roll
- Afternoon Snack: Apple slices with peanut butter
- Dinner: Baked salmon with sweet potato and steamed broccoli; side of brown rice
- Evening Snack: Whole grain crackers with cheese and a small orange
🎯 Key Takeaways for Pregnancy Nutrition
🥗 Eat the Rainbow
Include a variety of colorful fruits and vegetables to ensure a wide spectrum of vitamins and minerals.
🐟 Choose Safe Proteins
Prioritize lean meats, fish low in mercury, eggs, beans, and legumes for adequate protein intake.
🌾 Go Whole Grain
Replace refined grains with whole grains for more fiber, B vitamins, and sustained energy.
💧 Stay Hydrated
Aim for approximately 10 cups of fluids daily, primarily from water and water-rich foods.
🥛 Don't Skip Dairy
Include calcium-rich foods daily for fetal bone development and maternal bone health.
💊 Supplement Wisely
Take a prenatal vitamin as recommended by your healthcare provider to fill nutritional gaps.
📚 Sources & References
This content is compiled from the following reputable health organizations and medical guidelines:
- World Health Organization (WHO) - Nutrition Guidelines for Pregnancy
- Centers for Disease Control and Prevention (CDC) - Pregnancy Nutrition Information
- American College of Obstetricians and Gynecologists (ACOG) - Nutrition During Pregnancy
- U.S. Food and Drug Administration (FDA) - Food Safety for Pregnant Women
- Academy of Nutrition and Dietetics - Pregnancy Nutrition Resources
- National Institutes of Health (NIH) - Prenatal Nutrition Research
- March of Dimes - Healthy Eating During Pregnancy
- Cleveland Clinic - Prenatal Vitamins and Nutrition
- Institute of Medicine (National Academy of Medicine) - Dietary Reference Intakes
❓ Frequently Asked Questions
According to general guidelines, most women need no extra calories in the first trimester, approximately 340 extra calories in the second trimester, and about 450 extra calories in the third trimester. However, individual needs vary based on pre-pregnancy weight, activity level, and whether you're carrying multiples. Your healthcare provider can give personalized guidance.
Yes, fish can be part of a healthy pregnancy diet. The FDA recommends 2-3 servings (8-12 ounces) per week of low-mercury fish such as salmon, sardines, trout, and tilapia. Avoid high-mercury fish including shark, swordfish, king mackerel, and tilefish. Limit albacore tuna to 6 ounces per week.
According to the Academy of Nutrition and Dietetics, well-planned vegetarian and vegan diets can be nutritionally adequate during all life stages, including pregnancy. However, special attention is needed for nutrients like vitamin B12, iron, calcium, omega-3s, and zinc. Consider working with a registered dietitian to ensure your diet meets all requirements.
Most healthcare providers recommend prenatal vitamins even with a healthy diet because it can be difficult to obtain optimal amounts of certain nutrients—particularly folic acid, iron, and iodine—through food alone. Prenatal vitamins are designed to fill these gaps. Discuss the right supplement for you with your provider.
Morning sickness is common, but if it's severe (hyperemesis gravidarum) and prevents you from keeping food or fluids down, contact your healthcare provider immediately. They can recommend treatments to help manage nausea and ensure you stay hydrated and nourished. In the meantime, try small, frequent meals of bland foods and stay hydrated with small sips.
The Institute of Medicine provides general guidelines based on pre-pregnancy BMI: Underweight (BMI <18.5): 28-40 lbs; Normal weight (BMI 18.5-24.9): 25-35 lbs; Overweight (BMI 25-29.9): 15-25 lbs; Obese (BMI ≥30): 11-20 lbs. These are general recommendations—your doctor will provide personalized guidance based on your health status.
🤝 Support Edwin Ogie Library
Your support helps us continue providing free educational resources to learners worldwide.
Moniepoint (Local Bank Transfer)
Account Number: 7061335913
Bank: Moniepoint Microfinance Bank
Account Name: EDWIN OGIE
Every contribution, no matter how small, makes a difference. Thank you for your generosity!

Comments
Post a Comment
We’d love to hear from you! Share your thoughts or questions below. Please keep comments positive and meaningful, Comments are welcome — we moderate for spam and civility; please be respectful.